Table of Contents
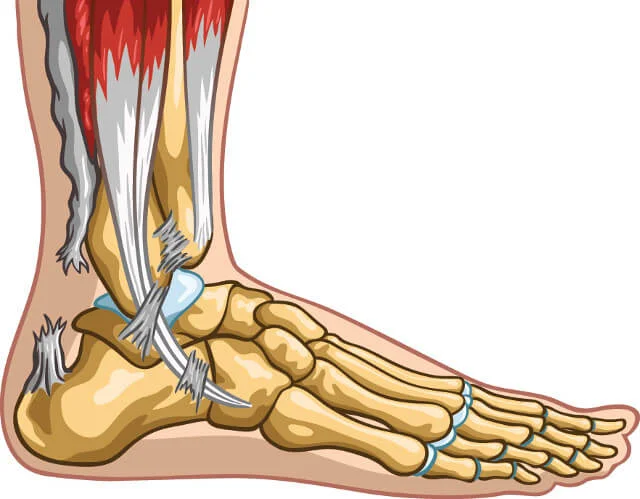
What Is the Achilles Tendon?
What Is an Achilles Tendon Rupture?
An Achilles tendon rupture is a partial or complete tear that occurs when the tendon is stretched beyond its capacity. Forceful jumping, falling, pivoting, or sudden accelerations of running, can overstretch the tendon and cause a tear.
Achilles tendon ruptures are most often seen in athletes. The “weekend warriors”, middle-aged people participating in sports in their spare time, tend to be the most prone to ruptures. Less commonly, illness or medications, such as steroids or certain antibiotics, may weaken the tendon and contribute to ruptures.
Signs & Symptoms
A person with a ruptured Achilles tendon may experience one or more of the following:
- Sudden pain (which feels like a kick, shot, or stab) in the back of the ankle or calf
- A popping or snapping sensation
- Swelling on the back of the leg between the heel and the calf. In some cases, there is a noticeable divot or deficit where the tear occurred.
- Difficulty walking (especially upstairs or uphill) and difficulty rising up on the toes
These symptoms require prompt medical attention to prevent further damage. Until the patient is able to see a doctor, the R.I.C.E. method should be employed:
- Rest. Stay off the injured foot and ankle, since walking can cause more pain, swelling, or further damage.
- Ice. Apply a bag of ice covered with a thin towel to reduce swelling and pain. Do not put ice directly against the skin.
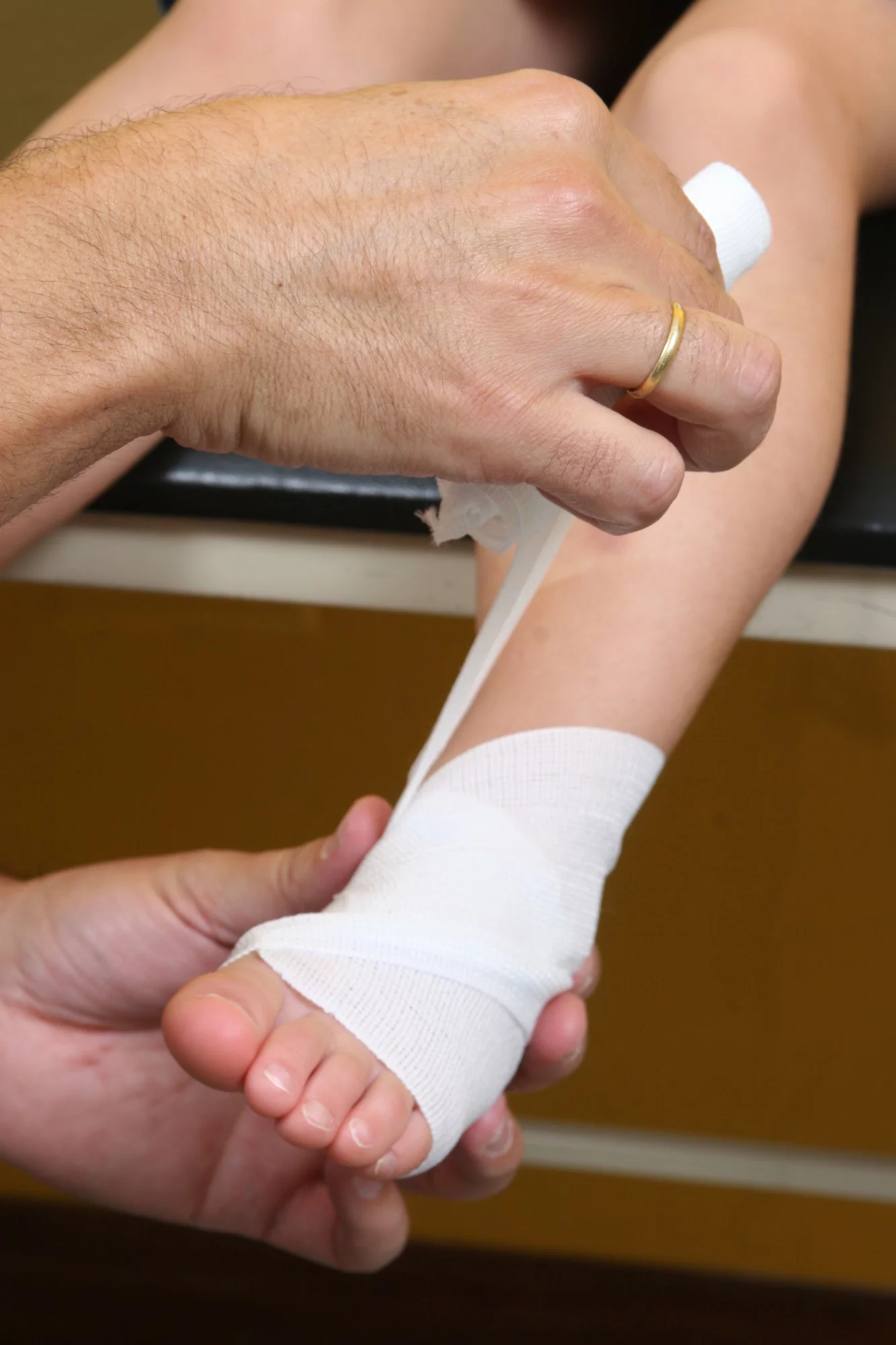
- Compression. Wrap the foot and ankle in an elastic bandage (ACE type) to prevent further swelling.
- Elevation. Keep the leg elevated to reduce the swelling. It should be even with or slightly above heart level.
Diagnosis
In diagnosing an Achilles tendon rupture, your doctor will ask questions about how and when the injury occurred and whether you’ve previously injured the tendon or experienced similar symptoms. Your doctor will examine the foot and ankle, feeling for a defect in the tendon that suggests a tear. Range of motion and muscle strength will be evaluated and compared to the uninjured foot and ankle. If the Achilles tendon is ruptured, the patient will have less strength in pushing down (as on a gas pedal) and will have difficulty rising on the toes.
The diagnosis of an Achilles tendon rupture is typically straightforward and can be made through this type of examination. In some cases, however, your doctor may order an MRI or Sonogram (Ultrasound). It’s important to note that MRI is the gold standard imaging technique to help assess the magnitude of this injury.
Treatment
Nonsurgical Treatment
Surgery
Surgery offers important potential benefits. Besides decreasing the likelihood of re-rupturing the Achilles tendon, surgery often increases the patient’s push-off strength and improves muscle function and movement of the ankle.
Various surgical techniques are available to repair the rupture. The surgeon will select the procedure best suited to the patient.
Following surgery, the foot and ankle are initially immobilized in a cast or walking boot. The surgeon will determine when the patient can begin weightbearing.
Complications such as incision-healing difficulties, re-rupturing of the tendon or nerve pain can arise after surgery.